Research, insight, and anecdotes behind an evolving body of advocacy on Vancouver Island
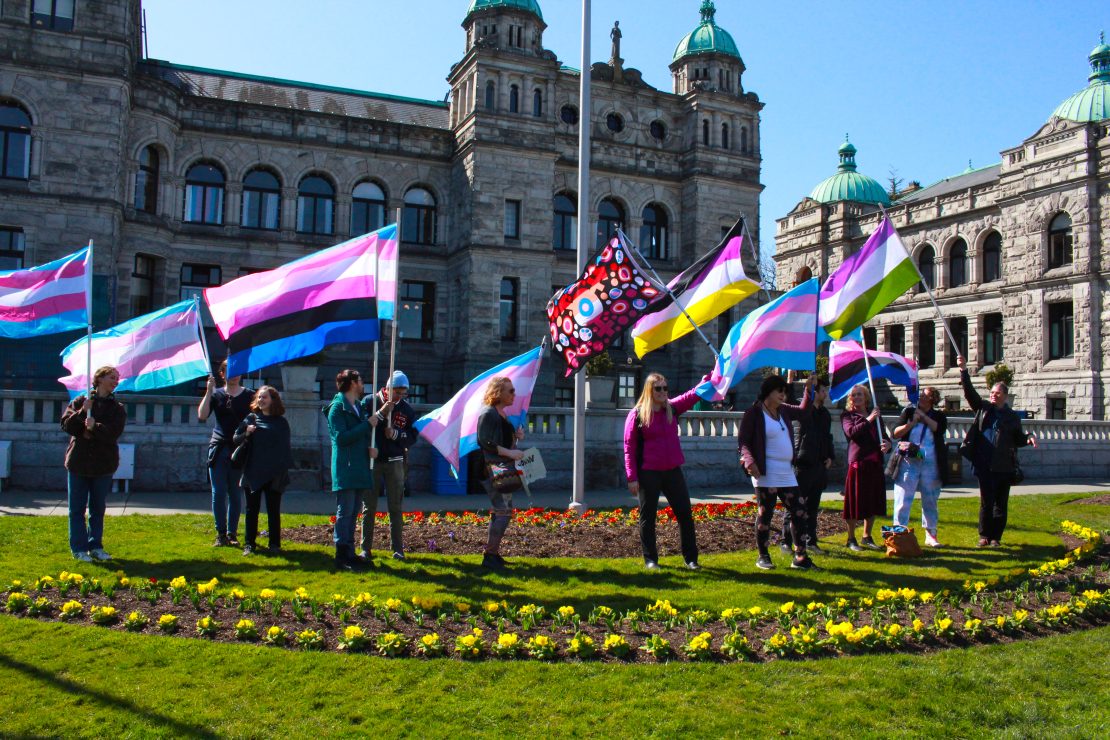
Photo by Maya Wei Yan Linsley.
It’s March 30 — just one day before the 14th annual International Trans Day of Visibility (TDOV). This year, the folks at Tau Wellness have kick-started the celebrations early with a visit to Victoria’s legislature.
The 10 of them arrive by water taxi, landing smoothly along the docks of Victoria’s harbour. Above, the skies are perfectly blue, but the city is unbearably windy. As they emerge from the boat, one by one, their flags unravel skyward, billowing out in clouds of pink, white, and blue.
In less than 24 hours, activists will call upon individuals across Victoria to pause, recognize, and celebrate the experiences of transgender, Two-Spirit, non-binary, and gender-diverse communities through space and time.
For the folks at Tau Wellness, however, TDOV transcends one calendar day. As anti-trans discrimination surges worldwide, communities on Vancouver Island are attempting to swing the pendulum back. While healthcare practitioners explore the creation of safer spaces within institutions, advocacy groups foster healing on the ground. Together, both are helping individuals explore intersecting experiences of gender identity and embodiment — every single day.
Grassroots advocacy
Tau Wellness, a community network of researchers, advocates, and healers, was originally formed as Rainbow Health Cooperative in 2014. The founding members, a small group of local activists, included ChrŸs Tei, who is acting director of the co-op today.
Tau Wellness’ formation was spurred, in part, by Trans PULSE, a community-based project aimed at addressing gaps in the health and well-being of trans and gender-diverse communities. Although Trans PULSE has since expanded nation-wide, the original survey, which was circulated in 2009, focussed exclusively on the trans community within Ontario. Then, between 2010 and 2011, Royal Roads professor Matthew Heinz conducted Victoria’s own needs assessment, which explored the experiences of trans communities on Vancouver Island.
These projects, both dedicated to understanding and improving the health and social needs of trans and gender-diverse people, were among the first of their kind in Canada — exploring the lived experiences of trans communities, by trans communities, for trans communities.
As a result of Heinz’s survey, around six community activists, including ChrŸs Tei, came together and decided that Vancouver Island needed a resource centre, one that would build a network of connections between an otherwise isolated group of individuals.
Initially, the team envisioned a gathering hub for community members to connect, build relationships, and foster a sense of belonging. Until 2017, their work was focussed solely on community support groups, funded straight from their pockets.
“We always did it with just the nickels and quarters we dug out of the sofas,” ChrŸs Tei recalled. “We just kind of went hand to mouth and got little bits of money.”
However, over the last decade, as research and awareness has shifted, so have the co-op’s goals. Around 2018, thanks to funding and further research opportunities, Rainbow Health Cooperative began its reorganization into Tau Wellness. Correspondingly, the co-op’s outreach has developed to include evidence-based, practice-proven community services.
An evidence-based approach to outreach
The transition to Tau Wellness began in 2018 with a grant from the Canadian Institute of Health Research (CIHR). ChrŸs Tei used this funding to form Our_Community Health Initiative (O_CHI) with UVic associate professor Nathan Lachowsky. O_CHI began as a five-year community research project, facilitated in partnership with the Victoria Native Friendship Centre, to explore the state of gender-affirming healthcare, and whether it was improving, across Vancouver Island.
In 2019, while acting as a Community Lead for O_CHI, ChrŸs Tei helped promote the second instalment of the Trans PULSE project within B.C. While Trans PULSE’s first project had explored the experience of being trans and transitioning in Ontario, the new study was larger — focussing on the health and well-being of trans and non-binary people across the country. This expansion was an integral step to protecting the human rights of trans and gender-diverse communities, both through policy and practice.
“Over three years, [the project was] basically looking at the care and lack of care that trans folks go through,” said Tanille Geib, current co-manager of Tau Wellness. “And how we could come up with bringing that information to community and medical health professionals.”
Last year, O_CHI was topped up with a Momentum Grant from the Vancouver Foundation, alongside additional support from the Victoria Foundation. Over this time, ChrŸs Tei has employed systems change investigation and participatory action research. Both models intend to tackle the root cause of social issues by taking a step back and working with communities to disrupt the major systems perpetuating inequities in the first place.
- Tau Wellness members. Nicola. Photos by Maya Wei Yan Linsley.
- ChrŸs Tei.
- Connie Quayle.
- Alex.
- Tanille Geib.
Creating self-sustaining community networks
By engaging in systems change investigation and collaborative research, ChrŸs Tei and her team were able to develop a more specific basis for their outreach, which effectively marked the transition to Tau Wellness. More recently, the co-op has shifted their work away from conventional research studies, towards reciprocal, community-based workshops, with a focus on preventing, healing from, and reducing symptoms of trauma.
“[Creating] safety and a space for the group of people that’s involved in this community is way more complicated than normal,” noted ChrŸs Tei, describing the intersections of trauma — and how to heal from them — in trans folks’ lives. “It takes a lot of work to get to that point, so the shift that we’ve been going through has been more centering around that reality in the community.”
In the latest stage of their outreach, the team at Tau Wellness is piloting a community wellness service that provides monthly, cross-generational, trauma-informed care, including prenatal workshops, paint nights, and community lunches. The goal of these support groups is to foster community resilience, while introducing individuals to self-sustaining healing modalities outside of the healthcare system.
“We’re wanting to train, and support, and nourish trans folks so they can be healers in their own communities … I think that’s a really powerful shift,” explained Geib. “Yes, we’re services based, and we do a lot of different projects, but it’s really about giving skills and tools to the community so that they can care for themselves and each other.”
Embodied healing
Connie Quayle, who recently began working with Tau Wellness, is on her own healing journey. As she navigates the twisting currents of complex post-traumatic stress disorder (C-PTSD), healing from the emotional upheaval associated with traumatic events, Quayle has begun exploring how she embodies gender and the role it plays in her life.
“There’s so much to transitioning, and embodying, and feeling, and tuning into yourself,” said Quayle. “Especially if you’ve had to pretend to be something different for so long.”
Serenely, Quayle recalls her physical transition, describing the moment she was able to step into herself for the first time — to embrace her body in all its beauty, rather than dissociate from it. She learned to channel this embodiment further through ecstatic dance workshops, and now with Tau Wellness, helping others explore how they hold gender in their own bodies and lives.
“I think it’s a pretty powerful experience,” said Quayle, regarding the rhythm and movement channelled through ecstatic dance and gender embodiment. “Lots of cis, and transgender queer folk have expressed the same throughout the workshop.”
For Quayle, healing goes beyond physical processes and surgical intervention. It transcends the body and represents more than a mere absence of disease.
“Healing is what we do when we’ve been traumatized. It’s what we do when there’s a break in the integrity of our bodies, or spirits, or hearts, or minds,” shared Quayle. “I’m talking about healing of the self, but in a way, that’s exactly what healing of others is.”
Quayle says, other than procedures that are purely physical, the healthcare system has little to do with healing.
“There’s often a time where we don’t get to express who we are,” said Quayle. “And when we do begin to transition and express who we are, there’s a huge loss of community, loss of privilege, income, job stability, housing stability, et cetera.”
According to Quayle, those losses are compounded by biases within the healthcare system, which often drops individuals as soon as gender-affirmation surgeries and hormone therapy are complete.
“It’s a trauma system of medical care, you know, it’s wartime medicine. It’s cut people open, patch them together, send them on their way,” explained Quayle. “But it ignores the experience of actually being trans … You’ve had a bunch of surgeries, you’re on new hormones, now what?”
Traumatization and treatment in numbers
As the psychological impacts of discrimination have been realized, researchers and advocacy groups around the world have focussed further on the link between transphobia and PTSD. Despite the persistent gap in research regarding trans experiences, ample anecdotal evidence and community-based research proves that there is a link between persistent transphobia and the intrusive thoughts, intense distress, and hopelessness associated with trauma.
In 2011, a national survey conducted in the U.S. compiled reports from 6 000 transgender individuals, 63 per cent of whom had been subjected to “an emotionally or life-impairing experience of discrimination.” Within Canada, Trans PULSE reported that 77 per cent of the transgender individuals surveyed in Ontario had seriously considered suicide in their lifetime and that individuals experiencing higher levels of transphobia were at greater risk of suicidal ideations.
Many gender-diverse people fight discrimination and harassment that is fueled by transphobic hate, stigma, and misinformation every single day. In Trans PULSE’s survey from 2019, most respondents reported experiencing verbal harassment related to their gender identity and expression at least once in the past five years. Over that same time period, 16 and 26 per cent of respondents had experienced physical violence and sexual assault, respectively.
As a result of pervasive discrimination, 64 per cent of respondents reported avoiding three or more public spaces (out of a list of 14 predetermined locations) for fear of being harassed or outed. These fears impact an individual’s ability to achieve adequate health and well-being, proven further by 45 per cent of respondents who reported having one or more unmet healthcare needs in the past year and 12 per cent who avoided the emergency room in the past year, despite needing urgent care. These numbers stand in stark contrast to the four per cent of the general population who reported having one unmet medical need in 2016.
“Trauma and transness — that huge intersection, it happens … not because there’s anything inherently connected about transness and trauma,” Quayle said. “But there is something connected about how trans people are treated in this world, in this day and age, that is traumatizing.”
A health practitioner’s perspective
Kirstin McLaughlin, the chair of Camosun’s nursing program, dedicates her research to culturally safe care of 2SLGBTQIA+ clients, attempting to fight the forces that traumatize clients within healthcare. McLaughlin describes the pervasive erasure and exclusion of queer identities that she’s witnessed in her own practice, everyday forms of bias that, although seemingly harmless, deem the healthcare system an unsafe space for trans communities.
“Within healthcare, we often ask questions of trans and gender-diverse people that are inappropriate,” described McLaughlin. “Because it’s really not directly related to the clinical care that we need to provide.”
Often, these questions are rooted in heteronormativity, as per the American Psychological Association’s definition: “the assumption that heterosexuality is the standard for defining normal sexual behaviour.”
As an openly queer person, McLaughlin has had health practitioners ask whether her partner was her sister, her cousin, or her friend, a question that, simply put, is irrelevant.
“This really forces queer folks to be in a position where they either have to out themselves or sort of dismiss the transgression,” said McLaughlin.
Further biases are rooted in cisnormativity, an ideology that assumes that most, if not all people’s natural gender identity matches the biological sex they were assigned at birth.
“The most blatant example is [that] a lot of our intake forms put sex or gender — because they’re often also conflated within healthcare — in the binary,” explained McLaughlin. “You tick off a box that you’re either male or female, with no real context.”
These assumptions actively work to erase the experiences of trans individuals and the 2SLGBTQIA+ community as a whole.
“The oversimplification and medicalization of sex and then the assumption that sex is the same as gender,” said Quayle. “That’s a huge error, a huge omission, a huge erasure of trans people within the medical system.”
According to McLaughlin, since individuals in Canada are tracked using their name and health number, this stigma follows them through every experience within healthcare. “Unfortunately, this can also reinforce use of folks’ dead names, which is very harmful,” McLaughlin added.
A history of exclusionary practices and discrimination within the healthcare system has led to a sense of distrust among 2SLGBTQIA+ communities. Therefore, creating a safer space for queer clients — in an institution they’re inherently excluded from — requires action to ensure the following questions, posed by McLaughlin, don’t need to be asked: “Do I trust the healthcare system? Do I trust my care providers? If I don’t, am I going to disclose my sexual orientation? Am I going to disclose my gender identity? Or does that potentially represent a lack of safety or something that could cause harm?”
According to McLaughlin, rather than ask these questions and risk the consequences of being wrong, many members of 2SLGBTQIA+ communities will delay or avoid seeking care instead, as seen in Trans PULSE’s survey results.
To unsettle this trend, McLaughlin believes that it is the inherent role of healthcare providers to maintain safe care, systems, and institutions, so that people will seek and receive appropriate care when they need it. From an educational standpoint, this requires constant dialogue regarding the systemic and structural barriers that queer communities face in healthcare, as well as the impacts those barriers have on collective health. Within institutions, McLaughlin believes that spaces must be carved out for trans and gender-diverse students to learn, which also means ensuring they’re accurately represented within the curriculum.
“We can normalize bodies other than bodies that we’re perhaps traditionally used to seeing,” proposed McLaughlin. “We can think a lot about language — and language as a site of power.”

Photo by Maya Wei Yan Linsley.
Student experiences
One nursing student at Camosun College has experienced the disconnect between intention and lived reality first-hand. Upon the student’s request, her name has been omitted from this story for personal privacy. Despite the inherent responsibility of nurses to provide safe care for everyone, regardless of identity, she often witnesses cis and heteronormativity emerge in class.
When learning about topics such as pregnancy, the student often hears instructors say something like “97 per cent of people giving birth are women, so I’m going to focus on that demographic.” she recalled. While they acknowledge that people other than women give birth, they choose not to focus on it.
This statement represents a common instance of cisnormativity, described by McLaughlin. In an education setting, by omitting the experiences of transgender men and gender-diverse people giving birth, healthcare practitioners risk contributing to the same stigmas that marginalize and traumatize those communities within the healthcare system.
Even when instructors do bring these discussions up in class, the student often witnesses biases seep into the room.
“I know people who … have scoffed at the word ‘chestfeeding’ because they think that [breastfeeding and giving birth] is a women-only process,” she explained. “Considering the [stigma] you see in the classroom already, if someone were to become a labour or delivery nurse, there is no way I would feel safe getting care from many of them.”
The lack of education around gender-diverse experiences, coupled with anti-trans bias in the classroom, leaves the student feeling scared for the future.
“One of the standards that we have to uphold is evidence-based practice,” she explained, a problem-solving approach based on the conscientious use of current research, clinical expertise, and client preferences. “It’s not being reflected … how are we learning if we’re using data from two years ago, and how are we incorporating [values] into our practice if our opinions clash?”
Going forward
The last decade has seen no shortage of resources aimed at improving care for queer communities. Whether that be through a day dedicated to trans visibility, an influx in nation-wide surveys and census data on gender-diverse experiences, or the steps that local educators and advocacy groups take every day to foster strength and community resilience — on paper, we’ve come a long way.
However, pervasive stigma subverts legal realities, showing that policies don’t always reflect the lived experience of those they intend to protect. Therefore, fostering a sense of belonging that transcends basic safety goes beyond mere legal amendments. Sustaining change day-to-day requires real, tangible action from each and every person.
For allies, this means remaining visible, taking action, and standing with marginalized communities, not only in fighting systems of stigma and transphobia, but in celebrating resilience as well.
“We all need to be examining the places and spaces in our lives where we occupy and have unearned privilege, and the ways that we contribute to the status quo without perhaps always consciously realizing that we do,” said McLaughlin.













